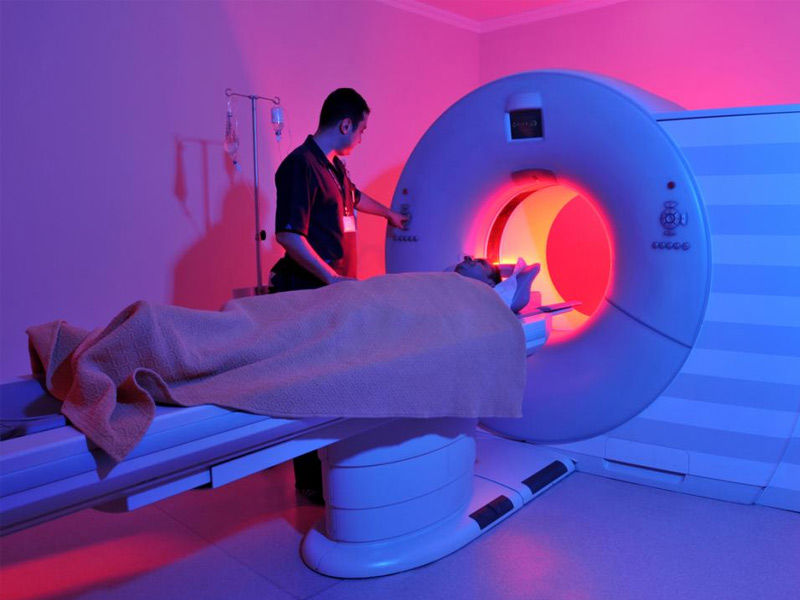
A slipping ruptured, or bulging disc is another name for a herniated disc. It ranks among the most frequent causes of the leg, back, and neck pain. In many cases, slipped discs recover on their own, but they need proper treatment.
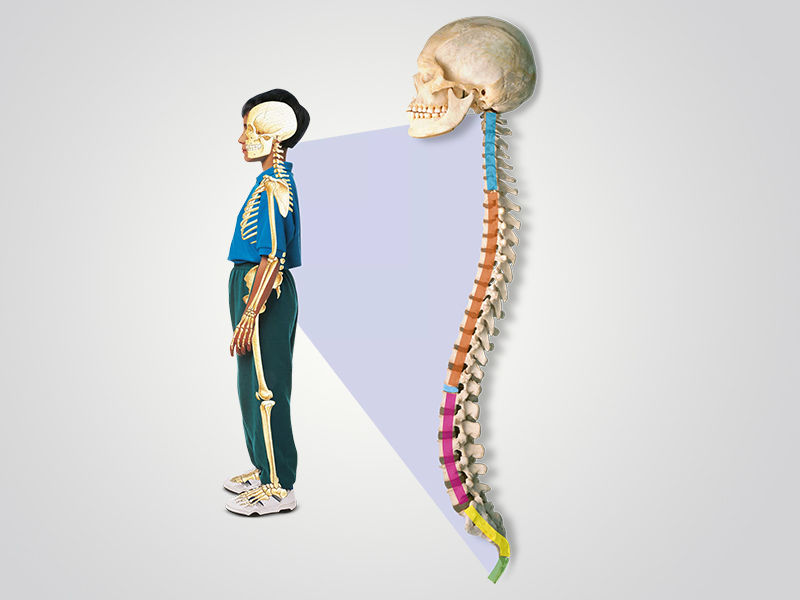
A herniated disc is what?
A herniated disc is a spinal injury (backbone). Your spine is made up of several bones called vertebrae that go from the base of your skull to the base of your tailbone. Discs are rounded cushions that sit in between your vertebrae. The discs separate your bones from one another, making it easy for you to bend and move. When one of these discs ruptures or starts to leak, the result is a herniated disc.
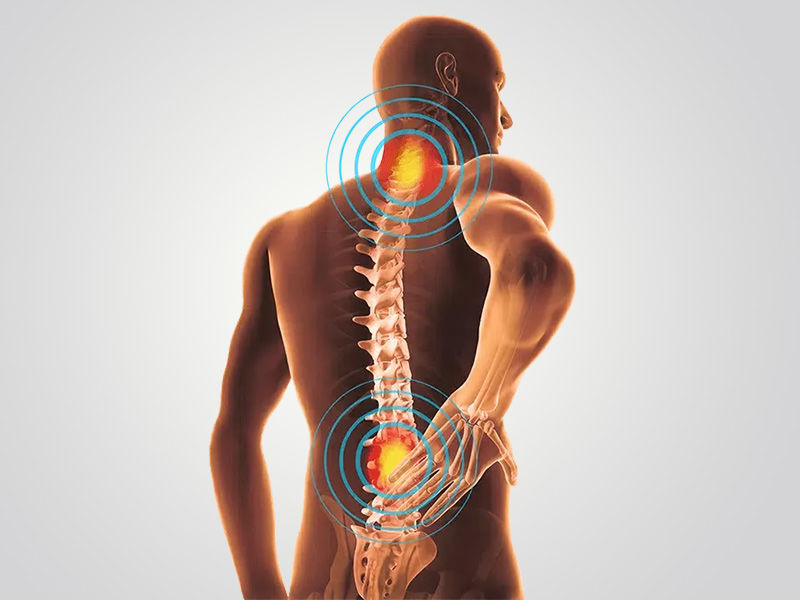
Herniated discs: are they common?
Although they can develop anywhere along the spine, herniated discs typically occur in the neck or lower back. It’s unusual to have a herniated disc in the middle of the back. Every year, up to 2% of people get a herniated disc. Herniated discs are the most typical cause of discomfort in the neck, arms, back, legs, and/or feet (sciatica).
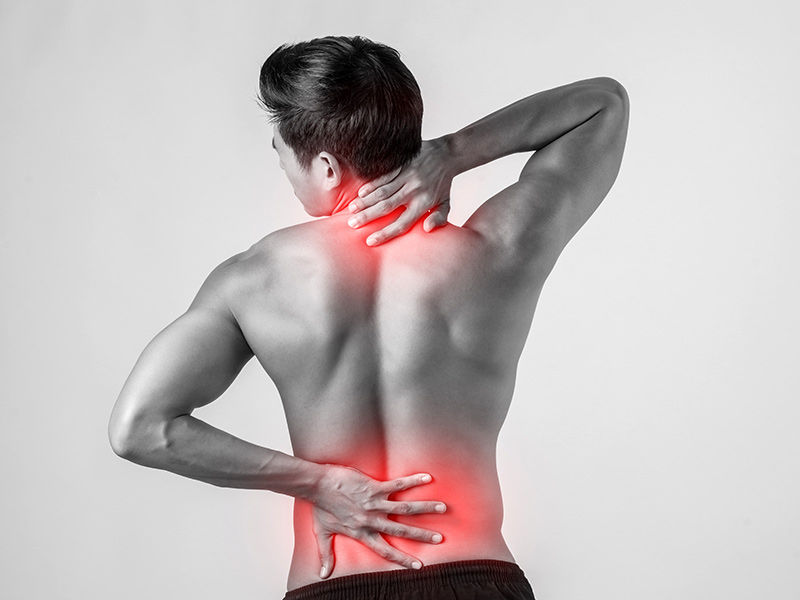
Those who have herniated discs.
The most prevalent age range for herniated discs is between 30 and 50. The problem affects men twice as often as it affects women. Other warning indications include:
- sitting still for extended periods.
- weighing too much.
- lifting large, hefty things
- repetitively bending or twisting for work, exercise, or recreation.
- smoking.
Why does a disc herniate?
Like a jelly doughnut, discs have tougher outer layers and soft, gel-like cores. The outer layer becomes more fragile and brittle over time. When the inner “jelly” material pushes through the crack, a herniated disc results. The adjacent spinal nerves may feel pressure from the leaky material.
A disc rupture can be caused by several reasons, such as:
- aging
- a lot of weight
- repeated movements
- abrupt tension brought on by incorrect lifting or twisting
What signs indicate a herniated disc?
Depending on where in the spine the problem is, a herniated disc presents with different symptoms. While rest improves symptoms, movement exacerbates them.
In the back, a herniated or slipped disc (herniated lumbar disk).
Slipped discs also cause “sciatic nerve” pain. Other indications of a ruptured disc in your lower back include the following: An abrupt discomfort that starts on one side of your buttocks usually radiates to a leg and, rarely, a foot.
- backache
- numbness in feet
- muscle sluggishness
- neck disc or herniated disc (herniated cervical disk)
Neck herniated disc symptoms include the following:
- If your problem is slipped disc you may also feel pain in your shoulder, arm, and even your hand and fingers.
- neck discomfort, particularly in the back and sides.
- tingling or numbness in your arms.
What can I do at home to ease the discomfort of a herniated disc?

- A herniated disk’s pain typically subsides with time. While your disc is healing, you can:
- If the pain is severe, rest for one to three days, although you must avoid spending too much time in bed to avoid stiffness.
- Use an over-the-counter analgesic, such as acetaminophen or ibuprofen.
- Heat and cold therapy are also very helpful.
What is the most effective slipped disc therapy?
If your symptoms don’t seem to be improving, you might need more sophisticated therapies. Your healthcare professional might advise:
Meds: Your doctor might suggest using an anti-inflammatory pain medication or painkiller.
Physical therapy: To assist reduce strain on your nerves, a physical therapist offers you an exercise regimen. Exercise helps to increase circulation and relax tense muscles.
Spinal injections: Also known as an epidural or nerve block, this procedure involves injecting a steroid medicine right into your spine. Medicine will reduce swelling in the muscles caused by a slipped disc.

Surgery may be necessary if a big herniated disc damages the bladder or bowel nerves. That might necessitate urgent surgery. When other therapies are unsuccessful, surgery is an option for non-emergency conditions.